Indian doctors fighting war against COVID ‘overwork, stress, fear’ | Coronavirus News Plague

[ad_1]
Low wages, 24-hour exchanges and a sharp decline in staff and self-defense equipment have left many doctors ahead of the recent epidemic in India as they fear for their lives.
Coronavirus has killed at least 165,000 people in much of South Asia – home to some of the world’s most populous cities – since early April.
Although India’s most recent operation on COVID-19 has declined recently, about 3,000 people are still dying every day and low-income payment methods are severely restricted.
“We’ve been working hard, we’re worried and we’re very scared,” Radha Jain, a doctor at New Delhi’s headquarters, told AFP.
The Indian Medical Association says more than 1,200 doctors have died from COVID-19 since the outbreak, plus more than 500 in the past two months.
Deependra Garg, a doctor who works near New Delhi, knows for himself how things have gotten worse.
His wife Anubha, 48, a medical doctor, was diagnosed with COVID-19 in April.
He started receiving treatment at home but as his condition worsened, he, like many other families, struggled to get to the hospital.
They later found about 200 miles from their home. But Anubha, who received the full vaccination, died within two weeks, leaving behind his 12-year-old daughter.
“We are ahead 24/7. We have a lot of HIV but we have to keep up the pressure because we have chosen this career, ”said Garg.
We are not free to choose. ”
Receive more money and stretch
The epidemic has exposed the weakness of the medical system in India, especially in non-governmental hospitals.
As the recent epidemic spread, reports came out of short hospitals for patients lying on the floor and sharing beds in overcrowded rooms, as relatives were protected by only cotton masks caring for their grieving loved ones.
The government spends less than 2% on gross domestic product (GDP) on medical care, one of the lowest in the world.
India had only 0.8 doctors per 1,000 people in 2017 – about the same rate as Iraq, according to the World Bank. The other two countries most affected by coronavirus, Brazil and the United States, had 2.2 and 2.6 respectively.
A pre-epidemic report from the Center for Disease Dynamics of America, Economics and Policy states that India needs another 600,000 doctors and an additional two million nurses to meet their needs.
Dr Shekhar Kumar, working with a private hospital in northern Uttar Pradesh, said young staff and graduate medical students sometimes had to work 24 hours a day.
“Compared to last year, this time patients need more time in the hospital which adds to the stress on staff,” Kumar said.
He also said that he had grown up again when his friends became ill with the virus.
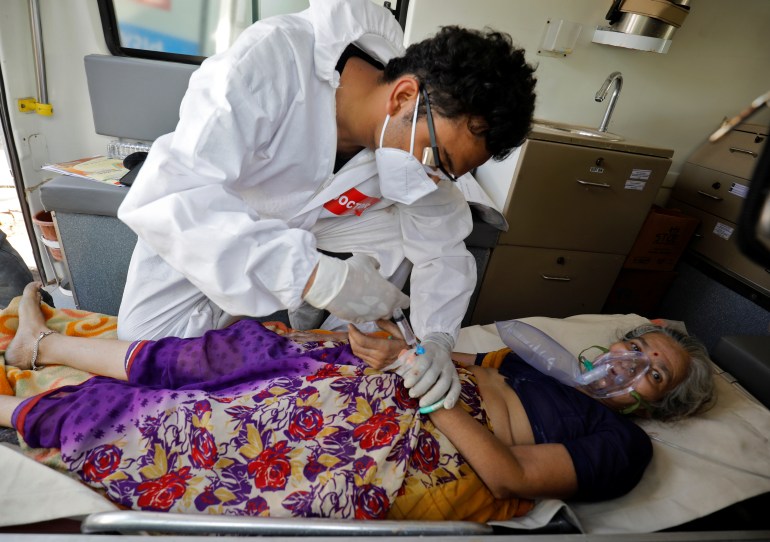 A doctor caring for a patient inside an ambulance waiting to be admitted to a COVID-19 hospital in Ahmedabad, India [File: Amit Dave/Reuters]
A doctor caring for a patient inside an ambulance waiting to be admitted to a COVID-19 hospital in Ahmedabad, India [File: Amit Dave/Reuters]
Doctors said they were disappointed by the pressure to select patients who should be rescued first due to complications with medication and oxygen.
Ravikant Singh, founder of the COVID-19, a charitable organization that helps set up field hospitals for hospitals, said he had difficulty sleeping one night.
“It has been a life-changing experience for doctors,” Singh told AFP.
“The worst thing was … we couldn’t save many lives because of the lack of air.”
Even after completing the exchange, doctors said they were concerned about sending their families home.
Kumar said he always thinks about how HIV is “hiding everywhere and everywhere”.
“If doctors cannot save their (their) lives, how can they save the lives of others?” he said.
[ad_2]
Source link



