Covid treatment is here

[ad_1]
In early March 2020, Pfizer’s chief scientist was summoned to the White House to discuss the epidemic.
Mikael Dolsten did not talk about the vaccine that would later bring the company fame and fortune: instead, in the early days, he described how the drug manufacturer works in treating patients who developed Covid-19.
“We’ve found a cure — a cure — that we can think about. . . he has a good chance, with an interest in fighting Covid-19, “he told President Donald Trump.
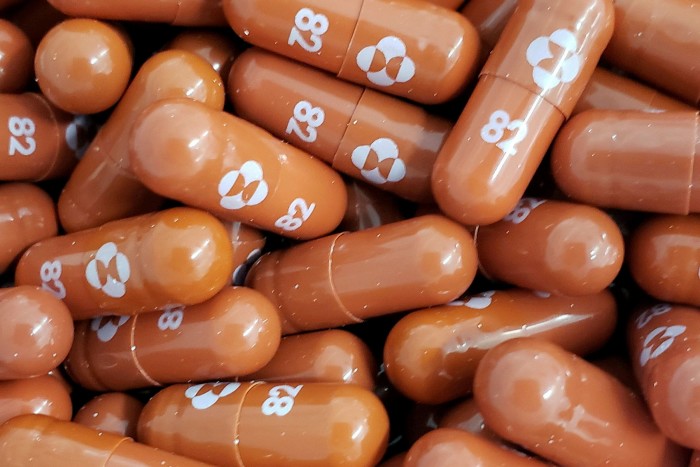
About 20 months later, Pfizer unveiled the first antiviral tablet designed to combat the Sars-Cov-2 virus.
Patients at high risk will soon have two new drugs that can change their care without even leaving them. Recent tests have shown that Pfizer tablets, called Paxlovid, reduce the risk of hospitalization and mortality by about 90 percent and drugs manufactured by Merck / MSD and Ridgeback Biotherapeutics reduce the risk of hospital stay in the middle. Merck drug, called molnupiravir, has received first approval, in the UK.
Oral antivirals will be an essential tool in medical care that seeks to reduce the number of Covid-19 patients this winter. Doctors have so far had to rely on expensive and difficult drugs to prescribe antiviral remdesivir in combination with antibodies, or drugs such as steroids that lower the body’s immune system after infection.
Daria Hazuda, Merck’s vice president for vaccination against infectious diseases, believes that “hospitalization is huge. . . Especially when you see surgeries and surgeries that seem to be taking place unexpectedly, with hospitals and health workers. [who] they just can’t seem to get their head around, ”she says.
Advertisers also believe that antiviral can speed up the recovery of the entire economy. Part 3 results of Pfizer raised shares in companies most affected by the epidemic, such as pilots and airline pilots.
However, this drug is not a cure. Most importantly, the results of the tests were for those who did not follow, while many in many countries will face fewer risks because of the shots. Given that the situation is still relatively small at first, there are questions about who should be the next, as well as concerns that developing countries are missing out on. Some scientists are also concerned about the side effects of patients or whether these drugs may encourage the virus to mutate.
Even health care providers who are happy to embrace the pills face difficulties in getting them to patients as quickly as possible. Carri Chan, a professor of health and pharmacology at Columbia Business School, says the pills are “very reliable”, compared to taking Tamiflu after the first symptoms of the flu.
“You can imagine, in the long run. . . when someone experiences symptoms, they go to a senior assistant or emergency care and get tested. After 30 minutes they have results and if they need treatment they can take it and go home, ”he said. “But I think we have to admit that we are still a long way from this.”
Repetition machine
Creating an antivirus is very difficult. Researchers should try to find a way to control the virus that does not infect the patient. Even so, the virus can adapt to drug resistance, so antiretroviral drugs (ARVs) are usually taken together. Kin-Chow Chang, a professor at the University of Nottingham who studies antibiotics, says that the production of these drugs is “more difficult” than vaccinating.
He said: “I am putting out a fire in an attempt to put out the fire.
Currently, Gilead remdesivir, repeated from a person who seeks to cure Ebola, is the main antivirus used in Covid-19. But it is intravenous, difficult to deliver at home or before people are hospitalized and there have been concerns about how they work.

Merck antiviral molnupiravir belongs to the same group of drugs. It interferes with the virus’ ability to multiply by triggering an explosion of virus in the virus, which in turn prevents the virus from working and spreading when it reaches a certain level.
In contrast, Pfizer treatment is a pill that blocks the protein that the virus has to replicate.
For some scientists, Merck’s therapeutic approach could lead to further complications. Ronald Swanstrom, a professor at the University of North Carolina School of Medicine, conducted animal studies that showed that the drug can accelerate DNA mutations within cells and that there is a hypothetical possibility that molnupiravir could affect human health.
“I think the use of this drug should be given to those who are most likely to have symptoms, who have symptoms and who are at risk. It should not be used to treat pregnant women, and we should follow the first-line treatment of long-term caregivers to see if there are side effects. , “says Swanstrom.
But Merck’s Hazuda criticizes the study as a “dangerous experiment” in which there is no consensus with small doses given to humans in the short term. Merck conducted several security discussions to understand the potential dangers, he said.
While there is no risk for each patient individually, we can all suffer if the mutations made in the drug have become too serious, warns virologist William Haseltine.
“These drugs cause the virus to change but if you don’t kill the virus then some can get out,” a former Harvard professor said.
But Hazuda said the risk of making the new changes increased because the virus had already done a good job of making the changes when they were allowed to roam.

Low pay
One of the possible problems is that antiviruses work best when given to patients. In the Pfizer trial, patients took their first pills within five days of starting symptoms. But it is still unknown how efficiency will decline at that time. Many scientists think that the first 48 hours will be necessary.
Health care providers may have difficulty prescribing these drugs to patients. Céline Gounder, an epidemiologist who worked on the Biden team of Covid-19 team, says the US health system is not set up to quickly identify and receive immediate medical attention.
“I don’t believe the drug is a game changer – not the way people think it will be,” he says.
Michael Mina, an assistant professor of epidemics at Harvard, says people at risk should be tested at Covid homes, which can be verified remotely and provided guidance by Uber. One US telemedicine project, eMed, is planning to send antiretroviral drugs to people with rapid test results.
“If you don’t have a test sitting in your closet waiting for you to use it, how many days does the average person go from smelling to downhill and getting tested?” asks Mina.
Perhaps the most difficult task will be to choose the one who will receive the least in a short period of time. Merck expects to have 10m training by the end of 2021, while Pfizer aims to create 180,000 courses by the end of the year and 50m by 2022.
Although both drugs have been tested in non-vaccinated individuals, the effects of these drugs may be seen to be very small in vaccinated individuals. Some antiretroviral drugs developed by Roche and Atea Pharmaceuticals were not able to reduce the number of viruses that people had as a placebo group after studying in a mixed vaccine and mixed group.

Pfizer is studying the treatment in vaccinated individuals but has not yet published the results.
“If Paxlovid does not benefit vaccinated patients, this could cast doubt on the value of many Paxlovid products, which could be very expensive,” says Andrew Hill, senior medical research researcher at the University of Liverpool.
Researchers expect the companies to sell their products for about $ 700 for treatment. Craig Garthwaite, a professor of medicine and health services at the Kellogg School of Management in Illinois, says this seems like a “very good price” for reducing expensive hospitals but not for making sure the vaccine “does not get spoiled”.
Some generic products may also be beneficial. A recent major peer study published in Lancet Global Health found that low-dose antidepressant fluvoxamine also reduced the risk of hospitalization in high-risk patients.
Healthcare providers can prescribe the drug to those who do not have the vaccine, although the vaccine – rising from about $ 4 to $ 25 a dose – would be much cheaper.
Dominic Wilkinson, a professor of medical ethics at Oxford University, says this is a new approach to disputes that are well-known as people who are responsible for their illness – such as cancer smokers – should share the money.
However, he said it was “unlikely” that care would be changed depending on “whether someone is wearing a mask, is away from him or is following the rules”.
Vaccinated pigs
The rush for developed countries to find antimicrobial drugs is reminiscent of earlier Covid-19 vaccine agreements, which left the world looking for remnants.
The US has agreed to spend $ 2.2bn on approximately 3.1m Merk drug courses, and the UK has signed agreements with Merck and Pfizer on approximately 750,000 courses between the two. Japan, Australia and South Korea are among the countries with alliances.
Eric Topol, director of the Scripps Research Translational Institute in California, warns that the pills are “also being ridiculed by rich countries, like vaccines”.
However, the tablets are easier to make and distribute than to shoot. Merck has already signed a voluntary patent with Medicines Patent Pool, a UN-sponsored human rights organization, to promote the production of low-cost generic products in developing countries. Pfizer is in talks with MPP, according to people who are familiar with the talks, who say they are “hopeful”.
Speaking at an FT conference this week, Pfizer’s Dolsten said he hoped the tablets would be distributed evenly but said it would not be easy if “the company wants to”, encouraging the establishment of an international body for the system to work. for low- and middle-income countries.
“I rotate my fingers on oral contraceptives. . . that we can do better around the world, “he said.
[ad_2]
Source link



